Study population
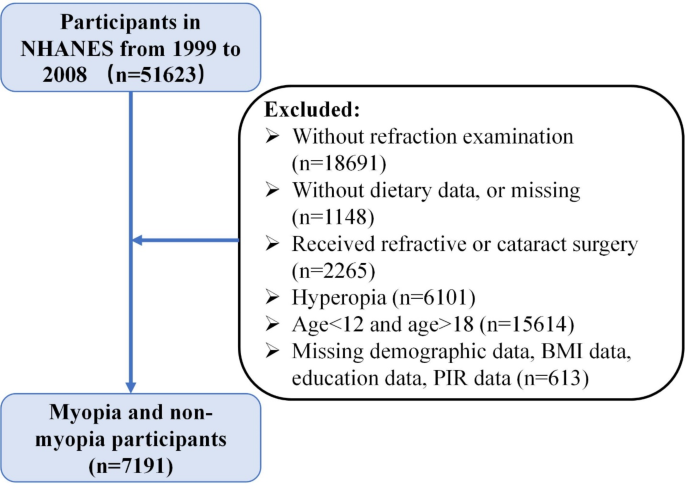
The NHANES is an ongoing cross-population-based survey to collect a plethora of information on the nutrition and health of the US population. Five cycles of data from 1999 to 2008 in the NHANES database were combined in this study, based on the availability of both refraction exanimation and dietary data. Participants who met the following exclusion criteria were included: (1) without complete data on refraction examination; (2) missing or without dietary data; (3) received refractive or cataract survey; (4) hyperopia that was defined as refractive error > 0.5 diopter (D) in any eye; (5) aged < 12 years or > 18 years; (6) missing demographic data, BMI data, education data and PIR data. Finally, the research comprised 7191 participants. The selection process is depicted in Fig. 1.

Flowchart of participants screening. NHANES, National Health and Nutrition Examination Survey; BMI, body mass index; PIR, poverty income ratio.
Assessment of myopia
All subjects aged ≥ 12 years were eligible to undergo objectively refractive measurements using an autorefractor/keratometry (Nidek ARK-760 A, Nidek Co. Ltd., Gamagori, Japan) in the non-cycloplegic conditions15,16. Average of three consecutive measurements were recorded for each eye. The spherical equivalent (SE) was calculated as sum of spherical error and half of cylindrical error. Because the two eyes of individuals were correlated, only the right eye of each participant was used for analyses15,16. Then, myopia was defined as SE value ≤ -0.5 diopters (D)17,18. Emmetropia was defined as the SE value between -0.5 D and 0.5 D, while hyperopia was defined as a refractive error > 0.5 D17,18.
Assessment of dietary inflammation index
Dietary intake data of NHANES participants were captured from the 24-hour dietary recall interview. To assess overall dietary inflammation, the dietary inflammation index (DII) was calculated. A total of 45 components were considered, and each parameter was assigned a specific DII score depending on their effects on six inflammatory biomarkers (IL-1β, IL-4, IL-6, IL-10, TNF-α, CRP). In present study, 26 nutrients out of 45 food parameters were used, including energy, protein, carbohydrate, dietary fiber, total fat, saturated fat, monounsaturated fatty acids, polyunsaturated fatty acids (PUFAs), cholesterol, vitamin A, β-carotene, vitamin B1, vitamin B2, niacin, vitamin B6, total folate, vitamin B12, vitamin C, vitamin D, vitamin E, iron, magnesium, zinc, selenium, caffeine, and alcohol. To evaluate the inflammatory potentials of each participant, firstly, we subtracted global standard mean from estimated intake of the individual, and then divided by the standard deviation. Secondly, Z-score value of each food parameter was measured and converted to centered proportions. Thirdly, each centered percentile was multiplied by the corresponding inflammatory effect index. Finally, the final score was summed for each participant. A positive DII score represents pro-inflammatory potential, while a negative DII score indicates an anti-inflammatory effect.
Assessment of covariates
To assess the influence of potential confounding factors, age, race, gender, education attainment, body mass index (BMI), and poverty income ratio (PIR) were taken into account. Majority of myopia appears during childhood and stabilizes by the age of 18 years19,20. Since visual acuity data of individuals aged 12 years or older were collected during NHANES21, it was not able to determine the relationship between DII and myopia in the children’s group. Therefore, we enrolled people aged 12–18 years, which seemed to be adequate. Furthermore, myopia in adolescents or young adults can be divided into early and late myopia using the age of 15 years as a cut-off point22,23. Then, all subjects were grouped into low age (12 to 15 years) and high age (16 to 18 years) groups. Race were divided into five categories: non-Hispanic white, non-Hispanic black, other Hispanic, Mexican-American and other ethnicities. The levels of education were designated as < 9th grade, 9-11th grade, high school grade, some college or above24. Three categories of PIR were identified: ≤ 1.3, 1.3–3.5, and > 3.5 25. BMI levels were classified as < 25 kg/m2, 25 to 30 kg/m2 or > 30 kg/m2 26.
Statistical analysis
Continuous variables were expressed as means with standard deviations (SDs), and categorical variables as frequencies and percentages based on the presence of myopia. To detect differences in baseline characteristics between myopia and non-myopia participants, variables were compared using Student’s t-test and chi-square test. DII scores were divided into quartiles from lowest (Q1) to highest (Q4), with the first quartile (Q1) being designated as the reference quartile. Multivariable logistic regression analyses were conducted to explore the risk of myopia with DII. The results were presented as odd ratios (OR) and 95% confidence intervals (95% CI). We estimated three models. Model 1 was a crude model adjusted for no covariate. Model 2 was a minimally adjusted model in which age and gender were first introduced (Model 2−1), and then age, gender, PIR, education level (Model 2–2). Model 3 was adjusted for age, PIR, education level, BMI, gender, race. Tests for trend were also performed with logistic regression. Additionally, subgroup analyses in terms of gender, age, race, education level, PIR, BMI were conducted to examine the presence of significant interactions of these covariates with the association between DII and myopia. Meanwhile, a smooth curve analysis was performed to elucidate the trend of the association between DII and myopia, where the DII score was treated as a continuous variable. DecisionLinnc software ( and GraphPad Prism were used for statistical analysis and figure design. Statistical significance was identified as a two-sided P < 0.05.
link