Choosing regional, rural, and remote practice: what attracts or deters early-career doctors? | BMC Health Services Research

A total of 25 junior doctors were interviewed from Townsville, Cairns, Mackay, and North West HHS (participation rates: 32%, 20%, 16%, and 32%, respectively). Over half were PGY1-2 doctors (52%), and the remainder PGY3-5. Most were female (76%) and under 29 years of age (84%). Based on Queensland Health internship priority classification, 15 participants were Group A, 4 Group B, and 6 were Group C or D. 68% of participants were graduates of Queensland medical schools, with 52% from James Cook University. While 33% were born in metropolitan areas, 67% were born in RRR settings. Regarding prior rural living experience, 60% had lived more than 10 years in a rural area, 20% for 5–10 years, and 20% for less than 5 years (Table 1).
Attractors
Analysis of the interview transcripts and reflective journals identified six categories referring to personal and professional reasons for choosing to train or work in RRR hospitals (Image 1). In this study, locals were defined as Queensland graduates, and non-locals as interstate or international graduate doctors. For non-local doctors, the decision to choose NQ was primarily restricted by the availability of options and regulatory rules. For Australian-trained doctors, the main motivators for rural training/ practice in NQ RRR hospitals were categorised as:
-
Regional hospitals: The “right size” (Participant Number (P)12- Regional [area of practice at the time of the interview]).
-
Family reasons (including friends and social network).
-
Experiencing something different (e.g., having an adventure or learning about medicine unique to NQ).
-
Recommendations from peers (and, also word of mouth).
-
Rural experience and intention.
-
Financial incentives.
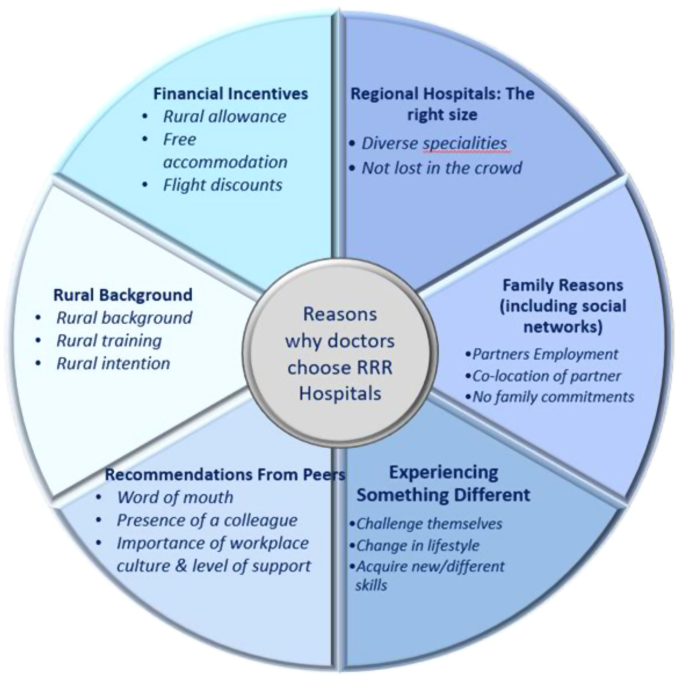
Attractors for choosing regional, rural or remote hospitals
Regional hospitals: the right size
Doctors referred to regional hospitals as the “right size” (P12- Regional), indicating that the hospitals were big enough to provide the clinical opportunities that the junior doctors needed while not being lost in the crowd of larger metropolitan hospitals. The hospitals also offered a mix of different specialities, but at the same time were small enough for junior doctors to become familiar with the system, and build and develop their professional network, especially for newly started interns looking to get the sense of a RRR context. [The italics indicate direct quotes from the participants].
I guess being familiar with the area and because It’s a tertiary hospital, so it has all the specialties. Even if I didn’t want to do surgery or radiology, I could still change my mind and still explore other options and then I think the other thing is that it’s not a big hospital where you don’t know your consultants’ name or the consultant never sees you. It’s big enough to have everything, but it’s still small enough for people to know you and for you to make good relationships that will be beneficial for like your future career. (P3- Regional)
Family reasons (including friends and social network)
Proximity to family, friends and social networks and being originally from or raised in RRR areas were frequently described as factors influencing the decision to preference RRR hospitals, “I’m from a city which is two hours from Townsville and my family is not too far. So, Townsville is like a second home… my parents come and go frequently. So, I want to be close to home, close to them.” (P1- Regional).
In couple relationships, the partner’s employment was repeatedly mentioned as a determining factor to stay, especially if the partner’s profession was considered as “niche” and specific to rural/remote areas, “I think the other thing that I think is important is having a partner- a partner who can find a job and have a job in regional rural areas and so both partners can stay and work there.” (P21- Rural).
The co-location of partners and the support from the hospital were recognised by the doctors and viewed positively. As this doctor described:
Other main factor was that my partner is an international medical graduate, and I had heard from friends and people that were above me, that Townsville really looked after those sort of couples and tried to give them both jobs and keep them together at the hospital, and so that was probably the main driving factor. (P22- Regional)
Experiencing something different
Doctors, especially those external to NQ, commonly said that one main reason for choosing a RRR facility was to challenge themselves, have an adventure or experience a lifestyle change. Exposure to populations from different demographic backgrounds was referred to as a special experience helping doctors get hands-on skills. Some doctors pointed to the potential for higher autonomy in RRR hospitals compared to busier and larger metropolitan hospitals. Learning rural clinical skills was an important factor; particularly, for those doctors who graduated from medical schools where undertaking rural placement was not a requirement.
New/different experiences meant different things to different doctors. For some doctors, moving across QLD HHSs provided an opportunity for exposure to different populations, “I wanted to challenge myself and move somewhere that would offer more experience in the early stages of my career. (P17- Rural)”, or similarly another doctor who mentioned, “So, we decided to come to [RRR hospital] because we had been in [RRR HHS] for three years, and I think [it] is a bit of a change… to see what the different health service was like…. I think… kind of experience-wise provides a very different population base.” (P7- Rural).
Recommendations from peers (word of mouth)
Participants spoke extensively about word of mouth being a key factor in their decision making when choosing RRR hospitals. Hearing firsthand about the facilities from a colleague who had already worked at a hospital was considered to be a reliable source of information. Further, the presence of friends/ colleagues in the destination hospital could potentially strengthen their decision to choose one of the NQ RRR facilities. Below are only a few example quotes:
I would say I was given lots of advice from doctors to stay in [RRR hospital]. It was doctors at the hospital here, but also at other places who said they’d recommend [RRR hospital] as a hospital. They told me to stay where I’m used to, or they worked there and they said it was really nice or even some people had moved away and said Oh I wish I’d stayed because it was really good. (P12- Regional)
Rural experience and intention
Some doctors who came from a rural background (e.g., born or lived in RRR areas) regarded rural work as a rewarding job, and chose NQ to make a difference in a rural community, “I’m brought up in this rural life background, I wanted to give back to my community. So, I thought to stay in [RRR town] and I was already familiar with the hospital.” (P1- Regional). Apart from the desire to serve rural communities, other factors were closely tied to doctors’ decisions to preferencing RRR hospitals. These included rural training and having background knowledge of the hospital, e.g., through their previous rural placements, “I’ve done a lot of placements out there as a medical student and then I was on the rural generalist pathway. So, [RRR hospital] quite fits in quite well with the rural generalist pathway because you get all your core rotations in the first two provisional years.” (P13- Remote). In addition to rural background or rural training, some doctors had the interest and intention of following a rural pathway, as this doctor described: “So, I’m thinking rural generalism, and thinking of applying to ACRRM [Australian College of Rural and Remote Medicine]. I’m like super keen on the rural generalist sort of job, work in a GP clinic and work in a hospital you know, you’re treating your neighbours and your friends and everything.” (P20- Remote).
Financial incentives
Rural allowance was appealing to doctors at different PG levels, and in particular to junior doctors who had planned to save money in the early years of their careers. Remuneration, rural allowance and free accommodation in rural and remote areas were referred to as “icing on the cake” (P13- Remote), indicating that they were probably not the main reason for rural-remote preference. The comments about rural allowance and accommodation were primarily made by doctors working in the Northwest Hospital and Health Service (NWHHS) sites that are classified as remote areas, with the MM rank of 6, “Obviously free accommodation was another big selling point as well as the rural allowance that you get, for going to work in [RRR hospital] as a junior doctor…That wasn’t the biggest selling point for me, but certainly a perk when I found out about it.” (P21- Rural).
Ten participants in our cohort were external to QLD, meaning that they were either interstate graduates, were on an international visa, or had received their medical degree from an international university, and therefore, were categorised as priority Groups B, C or D, respectively. Choice of the hospital for different priority groups could be restricted by certain legislative and regulatory factors that govern the recruitment process. For Australian-trained doctors, having rural service obligations, e.g. the Bonded Medical Program (BMP), and for groups C and D doctors being on an international visa were associated with some recruitment restrictions, which determined their choice of location of training/ practice. Some doctors in categories C and D, said that they used a scattergun approach to apply for multiple hospitals across the country, “I am [Nationality removed] and so with getting internship spots, I think we’re the third group or whatever to be assigned a spot. So, my chances of getting the spot at the regional Hospital are better than if there was other metropolitan site.” (P7- Rural). Similarly, another doctor said:
As an IMG [International Medical Graduate], we are not left with much choices. I think it’s just more of the situation we become in so we become in this situation… once we pass the AMC [Australian Medical Council] exam, so we just apply everywhere in Australia and whichever place gets back with the response, then we just focus more on to that place. (P24- Regional).
Barriers
This section summarises the major challenges the rural doctors reported in choosing or staying in RRR hospitals; some of these challenges were big enough for doctors to consider re-locating (Image 2). While many participants expressed a desire to serve rural communities, key barriers included:
-
Limited employment opportunities for rural generalists in RRR hospitals.
-
Inability to access desired rotations.
-
Social isolation and lack of community integration.
-
Poor workplace camaraderie.
-
High cost of living.
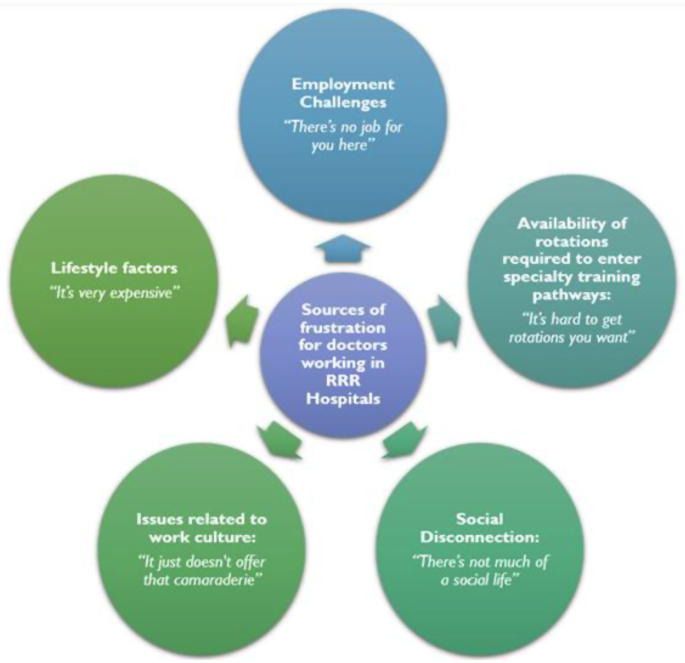
Barriers to choosing or staying in regional, rural and remote settings; RRR: Regional Rural and Remote
“There’s no job for you here”; employment challenges
Future employment emerged as a significant concern, particularly for Rural Generalist trainees in the rural and remote regions of North West, Mackay, and Cairns HHS. Despite completing both their Rural Generalist (RG) and Advanced Skills Training (AST) within these regions, many doctors struggled to secure positions aligned with their advanced skill sets. The lack of ongoing employment opportunities often forced them to seek work outside the region- or even outside the state. Employment was a common challenge in the North West sites, where the local hospitals focus is predominantly on training new doctors, rather than retaining existing trainees upon completion of their pathways.
I think one of the biggest consequences is that it [RRR hospital anonymised] is a specialist-led hospital, so you know, staff specialist, consultants in specific fields run each department. Because of that, there’s not a lot of senior positions for rural generalists at that hospital. So, a lot of people in my position do have to leave because even if they do all their ACRRM training there, they don’t hire rural generalists. (P13- Remote)
Some rural generalists described situations where after completing certain AST, they were upskilled to a point where they could no longer be hired by the same hospital in which they trained because there was no senior role defined for that type of skillset. The concern was, in part, because of not receiving a job offer and also not getting the chance to use the AST skills that they were trained for. As this doctor described, there was a concern about becoming de-skilled and moving backwards if not offered a relevant position:
There’s not really a role within the hospital to accommodate an advanced diploma that, like someone that’s got the certificate and has finished that training year. So, although I could have done GP training at [RRR centre] which is the GP clinic, there wouldn’t have been the opportunity for me to use the diploma by doing any inpatient obstetrics, which felt like will be a step backwards after finishing a year of the intensive training. (P17- Rural)
“It’s hard to get rotations you want”: availability of rotations required to enter specialty training pathways
Experiences were diverse regarding availability of rotations. Offering rotations that aligned with the doctors’ intended career pathway has the potential to keep the doctors satisfied, and act as an incentive for remaining at that hospital. But some doctors were unhappy if they did not get the rotations they wanted; in particular, if the doctors were on, or trying to get on, a specialty training pathway and had to complete certain mandatory rotations as part of this training. Accommodating doctors’ preferred rotations was frequently referred to as a key strategy for workforce sustainability, which could potentially benefit both local doctors and those considering a return to their non-metropolitan hometowns.
I would say it can be difficult to get the rotations that you want, especially if you’re in your PGY2 and 3…. you’re thinking of getting onto a special training program….
Rotations… That’s the reason that I’m not working at [RRR Hospital] this year, because I was on ACRRM and I needed paediatrics and anaesthetics and other things….
I did e-mail about it, I was like hey look like you know I’m on ACRRM program and I thought that I would get at least one of these… what’s going on?…. I was like why would I do another hospital-based rotational year if I’m not going to get the only two hospital-based rotations that I actually need? (P14- Rural)
“There’s not much of a social life”; social disconnection
Social life in RRR areas is different from that of bigger cities. Feelings of isolation were a recurring sub-theme regardless of the doctors’ gender or PG level. However, certain groups of doctors appeared to have had greater difficulties, including non-local doctors and those living without their family or friends nearby.
I think what’s hard is not having family close by, that’s even though I’ve been away from home for seven years at university, I think the actual distance from home makes it hard because you can’t just go visit family quickly and you often don’t have enough time off and you know at weekends not long enough to be able to go see them or to justify the cost of flights and things. So, I would say that would probably be the hardest. (P6- Regional)
Building a social network could prove difficult for non-local doctors, especially young interns, who came to a new environment and started a professional life, with limited time to make friends outside of work.
For most people it would be coming into a new town, and building your social network again, and that’s happened probably slower than what I’m used to, given that at university it’s quite easy, and then as soon as you’re in a professional environment, it’s not as easy to build those social connections outside of work, given how busy everyone is, and also, I think we’re all tired at the start of internship, which kind of makes it a bit harder and a bit more effort required. (P6- Regional)
The same doctor, who did her medical degree in a metropolitan area, referred to limited “outdoorsy” events and café culture in RRR areas which could potentially limit doctors’ ability to socialise outside the hospital and mentioned, “I think a lot of the time when I’ve spoken to others, they reminisce about food in Brisbane or food in Melbourne and going down and doing stuff like that” (P6- Regional). Another doctor, who also came from a metropolitan area, referred to the “transitory culture” (P5- Regional) of the medical workforce in RRR areas, and the fact that the non-locals often prioritise work over family, even if it is not what they wish to do, “They get ticked off what they need and then they go. If you’re not from here, it’s rare that you’ll want to stay because …. for a lot of people, even for people who don’t necessarily want to have it this way, work is the priority, because there’s nothing else, in terms of like just activities and things to do.” (P5- Regional).
“It just doesn’t offer that camaraderie”; issues related to work culture
This sub-theme discusses the challenges related to the hospital departments, or the relationship that doctors had with their seniors, supervisors or other hospital staff. A lack of trust between staff in some departments was a push factor for moving out. The majority of doctors spoke about the supportive environment in the hospitals in which they were working. They compared the RRR environment favourably with the metropolitan hospitals based on their own previous experiences or from second-hand information from their colleagues, and expressed satisfaction with the level of support they received during their internship and subsequent years as a junior doctor. The doctors positively spoke about being “thrown in the deep end” (P8-Regional) from the early stages of their internship and referred to it as an opportunity for autonomous practice, which in the majority of cases was associated with proper supervision. For newly started interns, the experience could have been daunting at the beginning; however, too much responsibility early in their career did not appear to negatively impact their training experience as long as the responsibilities were accompanied by support from senior staff. However, some doctors also shared some experiences where they felt they were left unsupported and their call for help was not responded to appropriately. Some doctors expressed concern not only because of the loss of training opportunities, but because of patient safety. One doctor called the hospital environment “adversarial” and shared: “[RRR hospital department] was one of the ones that just made me like, do I even want to do Medicine, if this is what it’s like… we weren’t getting support from the registrars or the PHO’s, so you just felt very unsupported in your decision making.” (P18- Metropolitan).
“It’s very expensive”; lifestyle factors
Costs of living, accommodation and flights were identified as some of the major financial challenges for junior doctors in RRR locations. These additional costs acted as a deterrent for doctors when making the decision to come to on or stay on in rural areas. As these doctors described, “Probably the biggest part was the cost of getting out of [RRR hospital]. The flights are very expensive even with the resident discount. It’s very expensive to get even just to [RRR town].” (P17- Rural).
A few doctors commented on the challenges associated with meeting the family’s needs and expectations in rural and remote areas; e.g., traveling, children’s schooling and access to veterinary services, “When their kids reach high school, if there’s not a lot of good schooling options in that area, they’ll often have to move to a city. Boarding school is very expensive. You know, it’s 50 grand a kid per year. So that’s even on a doctor’s wage, that’s not sustainable.” (P13- Remote). Access to health and welfare services could even be a challenge for the doctors themselves. It was acknowledged that such limitations may justify the fact that some doctors choose to fly in fly out rather than stay in the town permanently.
link

![Locum tenens offers physicians a path to freedom [PODCAST] Locum tenens offers physicians a path to freedom [PODCAST]](https://kevinmd.com/wp-content/uploads/Design-4-scaled.jpg)

![Sabbaticals provide a critical lifeline for sustainable medical careers [PODCAST] Sabbaticals provide a critical lifeline for sustainable medical careers [PODCAST]](https://kevinmd.com/wp-content/uploads/The-Podcast-by-KevinMD-WideScreen-3000-px-3-scaled.jpg)