A novel paradigm in cleft lip education: integration of 3D-printed simulator and problem-based learning | BMC Medical Education

Participants
A total of 40 stomatology undergraduates from the Medical Department of Wuhan University were enrolled in our study. Experienced educators were assigned as tutors in the teaching class. Students were randomly divided into two groups: the 3D-printed PBL group and the traditional PBL group, each comprising 20 students. The research subjects provided informed consents and agreed to participate in the study.
3D-printed cleft lip simulator
The 3D-printed cleft lip surgical simulator used in this study was commercially procured from Sckangming Company (Sichuan, China). It was fabricated based on patient CT imaging data through computer-aided design (CAD) to construct a three-dimensional model, followed by high-precision printing using silicone synthetic resin materials. These materials were selected for their high tensile strength, tear resistance, and compression set durability, enabling repeated surgical manipulations while maintaining structural fidelity [15, 16]. The silicone resin’s hyperelasticity and tactile feedback closely mimic tissue elasticity and deformation during surgery, critical for realistic skill acquisition. The simulator features multi-layered anatomical structures (skin, muscle, mucosal layers) and modular replaceable components to adapt to diverse training scenarios, as well as repetitive surgical instrument penetration, suturing, and traction. Due to proprietary technology and commercial confidentiality protections, specific technical details were not disclosed by the manufacturer. For comprehensive fabrication protocols, further validation requires access to proprietary technical documentation or authorized materials provided by the manufacturer. Comprehensive fabrication protocols require access to authorized materials provided by the manufacturer.
Traditional sponge models
The traditional PBL group employed low-density sponge models, a cost-effective material lacking anatomical stratification or biomechanical realism. Sponges exhibit homogeneous texture, minimal resistance to surgical instruments, and poor mimicry of tissue layers (e.g., skin-muscle-mucosa interfaces), resulting in unrealistic haptic feedback and limited surgical skill transfer. Their selection was driven by accessibility and historical use in basic procedural training, but their inability to simulate tissue tension, layered dissection, or dynamic deformation underscores their inadequacy for advanced cleft lip repair education.
Study design
The teaching process of integrating 3D-printed cleft lip simulators with the PBL method was employed in the 3D-printed PBL group. Conversely, the traditional PBL group utilized the conventional PBL teaching method. The chapter on cleft lip repair in the undergraduate textbook of Oral and Maxillofacial Surgery was selected as the teaching content. The two groups of students received comparable teaching environment conditions, including instructors, textbooks and equal learning hours. The teaching process is shown in Fig. 1.

Basic flowchart of the teaching process
3D-printed simulator integrated with PBL teaching method
In the initial phase, students in the 3D-printed PBL group were provided with an authentic clinical case (unilateral cleft lip) and a 3D-printed cleft lip simulator, which required collaborative exploration encompassing identification of anatomical landmarks within nasolabial subunits, quantitative morphometric analysis of deformity characteristics, and surgical approach formulation, followed by the creation of a Microsoft PowerPoint presentation (Microsoft Corporation) to synthesize and present their findings. During the PBL class, a representative from each group presented the PowerPoint. Members of the 3D-printed PBL team could pose inquiries regarding the selected cases and engage in discussions on various issues. During the case discussion, the instructor guided the students in highlighting the key points and challenges associated with the problems. In the subsequent operation link, the instructor introduced the anatomical characteristics of the orbicularis oris muscle, the severity of the deformity, and the surgical process using the 3D-printed cleft lip simulator. The instructor then provided a detailed demonstration of the surgical process (Figs. 2 and 3). Following the instructor’s presentation, the group of students utilized the simulator to practice the surgical procedure. As a facilitator and motivator of group learning, the tutor provided a summary and explanation of any remaining questions.

Representative images showing theoretical teaching and operation training sessions. A. Participants engaged in a 1-hour theoretical session led by clinical dentists, who were chief physicians with abundant practical experience in the field. B. The instructor elucidates the key components of unilateral cleft lip surgical procedures
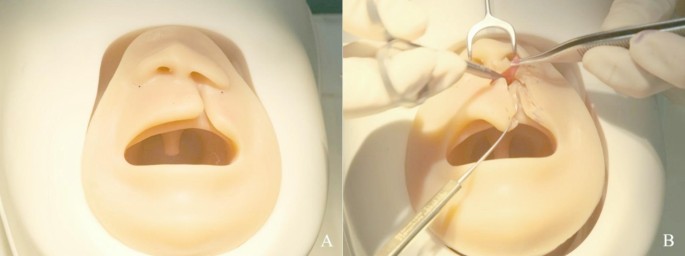
Unilateral cleft lip surgery simulator. A. The design and features of the cleft lip surgery simulator are demonstrated from an anterior view. B. A detailed view of the muscle tissue flap simulating the orbicularis oris muscle, highlighting the intricacies involved in the surgical procedure
Traditional PBL teaching method
In the initial phase, students in the 3D-printed PBL group were provided with an authentic clinical case and assigned learning tasks. During the PBL class, students initially presented their PowerPoint presentations and discussed encountered challenges, after which instructors delivered targeted theoretical instruction on cleft lip-related concepts using multimedia platforms. Subsequently, during the surgical simulation phase, instructors demonstrated standardized surgical procedures utilizing sponge models, while students practiced cleft lip reconstruction techniques on identical simulators to refine operative skills under guided supervision.
Assessment and feedback
Before class, examinations of students’ knowledge of cleft lip repair were conducted to establish a baseline understanding of their knowledge level. The detailed results are shown in Table 1. Following the completion of the training period, both groups underwent theoretical examinations. The assessment of cleft lip repair included a test of 10 questions, with 10 points for each question, resulting in a total score is 100 points. [See Supplementary Tables 1 and 2] Subsequently, we performed a section analysis of in-class theoretical test scores [17].
In the second phase, students were assessed through an operational test to evaluate their mastery of skills. The assessment of the surgical process comprised content from the Chinese Oral Physician Internship Course Exam. The evaluation was conducted by two professional doctors with five years of clinical experience. The items and scoring standards included surgical location, incision design, incision technique, and the effect of stitching. The operation assessment included a test of 6 questions, with 10 points for each question, resulting in a total score is 60 points. Within each scoring interval, the final score was determined based on the number of deviations and the magnitude of specific quantitative parameters listed in the table [See Supplementary Table 3].
Upon the conclusion of the Cleft Lip Course, we distributed a self-assessment questionnaire [See Supplementary Table 4]. The questionnaire comprises the following items: (1) Interest in learning; (2) Efficiency of learning; (3) Understanding of common surgical methods; (4) Improvement of clinical practice skills; (5) Understanding of the anatomical structure of the lips; (6) Understanding of fixed point design; (7) Understanding of muscle dissection and separation techniques; (8) Understanding of tissue rotation and alignment during suture; (9) Confidence in future cleft lip surgery; (10) Satisfaction with teaching methods. Each item on the Likert scale is assigned a score of 5 points, with the highest score being 5 and the lowest score being 1.
Statistical analysis
Data analysis was conducted using SPSS 25 statistical software (IBM Inc., Chicago, IL). Baseline scores were compared using a paired t-test. The In-class theoretical test scores were expressed as [M(P25, P75), points], and the Mann-Whitney U test was used for comparing the two groups. The operation assessments were compared using an independent samples t-test. The self-evaluation of comprehensive ability and satisfaction level with teaching methods were assessed using the Mann-Whitney U test, with a significance level of P < 0.05 indicating the statistical significance.
link



![Locum tenens offers physicians a path to freedom [PODCAST] Locum tenens offers physicians a path to freedom [PODCAST]](https://kevinmd.com/wp-content/uploads/Design-4-scaled.jpg)