Analysis of stress responses in medical students during simulated pericardiocentesis training using virtual reality and 3D-printed mannequin
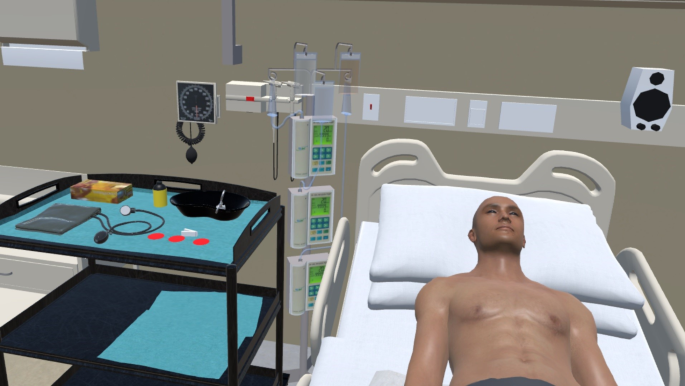
Our results suggest that VR is comparable to traditional mannequin-based training in simulating stress responses during pericardiocentesis. Although VR offers an immersive and interactive environment, our findings cautiously support its equivalence rather than its superiority over traditional methods. This aligns with research by Mergen et al., who noted the capability of VR in procedural training without conclusively establishing its enhancement of clinical decision-making skills13. These findings underscore the importance of integrating VR with complementary training approaches to achieve comprehensive educational outcomes.
In line with Bolton et al.’s findings, VR has the potential to enhance access to medical training in low- and middle-income countries14. However, to maximize its impact, broader applications must prioritize sustainability and adaptability to local contexts, addressing challenges such as infrastructure limitations and economic barriers. Additionally, as Weissglass highlighted, the integration of emerging technologies such as medical artificial intelligence with VR necessitates robust policy frameworks to mitigate biases and ensure equitable access15.
We explored the integration of 3D modeling with VR and demonstrated its potential to enhance both the cost-effectiveness and accessibility of medical training. This approach aligns with the findings from Roh et al., who emphasized the benefits of using open-source software and photorealistic 3D models in surgical training16. Such advancements hold relevance for resource-limited settings, where cost-effective and scalable solutions can significantly improve the reach and impact of simulation-based education.
We also examined the psychological aspects of medical training. By incorporating 3D-printed mannequins and VR, we addressed the technical and emotional challenges healthcare professionals face. Similar findings by Towers et al. highlight the value of such methods in fostering emotional resilience17. Further, Rochlen et al. reported significant improvements in student confidence and procedural accuracy using VR and 3D technology18.
The application of VR in critical care settings, as discussed by Bruno et al., highlights its potential to enhance educational outcomes, while presenting challenges related to technology integration, cost, and ethical considerations19. These insights underscore the need to navigate technical and human factors to fully exploit the benefits of immersive technologies in high-stake environments.
Our secondary analysis revealed significant interactions between stress parameters and demographic variables, including age, sex, lifestyle, and medication consumption. Younger participants (< 23 years) exhibited higher LF/HF ratios during the simulations, indicating greater sympathetic activation compared with older participants. This finding is consistent with Helman et al.’s study, which indicated that younger individuals, who often have less clinical exposure, perceive simulations as more stressful, leading to greater physiological responses20.
Interestingly, the use of anxiolytics was somehow associated with alterations in HRV parameters, such as higher LF/HF ratios, suggesting that baseline autonomic regulation may be affected in individuals using these medications. These findings emphasize the need to consider medical treatments when designing and interpreting simulation-based training outcomes, because such treatments may independently modulate stress responses, irrespective of demographic or experiential variables.
No significant differences in HRV metrics were observed based on sex, which contrasts with existing literature reporting higher self-reported stress levels in female participants21. This divergence highlights the importance of using objective biometric measures, which may provide a more reliable understanding of stress responses than subjective assessments alone.
In terms of lifestyle, family income and work-study balance significantly influenced stress-related physiological responses, underscoring the complex interplay between socioeconomic factors and stress. These findings align with prior observations, such as Kreutz et al.’s work on the effects of lifestyle changes induced by the coronavirus disease pandemic on blood pressure and hypertension, further illustrating the interconnectedness of lifestyle factors and health outcomes22. However, other lifestyle habits, including caffeine consumption and physical activity, did not exhibit significant associations with HRV in this study.
Finally, including HRV analysis in VR simulations provides a novel approach for assessing stress responses, which is critical in preparing medical professionals to perform effectively under pressure. This aspect of our study aligns with the findings of Corrigan et al.23, who emphasized the ability of VR to replicate and manage real-world stress conditions effectively24.
These insights emphasize the complexity of physiological responses to stress and underscore the importance of personalized training approaches that account for demographic, pharmacological, and socioeconomic variability. Designing simulations that address these individual differences can improve medical students’ emotional and technical preparedness across diverse learner populations.
Several limitations should be considered when interpreting these findings. First, participant recruitment was based on voluntary enrollment without a formal sample size calculation. Although the sample size was adequate to detect meaningful variations in stress responses, this convenience sampling approach may restrict the generalizability of the findings to a wider population. Second, the study was conducted in a high-income country, which limits the applicability of our results to settings with different economic and healthcare conditions. Moreover, the participant group was limited to final-year medical students, raising questions about the generalizability of the findings to other populations. For instance, first-year medical students, who typically have less clinical exposure and underdeveloped stress management skills, may exhibit heightened physiological stress responses in similar simulations. Conversely, practicing healthcare professionals, equipped with advanced coping mechanisms and greater clinical expertise, may display more stable autonomic responses and perceive these simulations as less challenging. Additionally, the focus on pericardiocentesis, a complex and high-stakes procedure, may not fully capture the range of stress responses encountered across different medical scenarios. For instance, less invasive tasks, such as basic suturing, are unlikely to elicit similar levels of physiological activation. In contrast, highly dynamic and time-sensitive interventions, such as trauma resuscitation and advanced cardiac life support, may trigger more pronounced sympathetic responses. Future studies should explore how simulation-based training impacts stress responses across a wider spectrum of medical procedures to optimize educational strategies for various clinical contexts. Finally, our focus on a single VR platform and a specific 3D-printed mannequin limits the generalizability of the findings to other training models or technological implementations. Future research should explore the applicability of diverse VR platforms and 3D-printing technologies in various educational scenarios to provide a more comprehensive understanding of their potential in medical training.
This study makes a unique contribution to medical education by directly comparing stress responses in two distinct simulation modalities—VR and high-fidelity mannequins—within the context of pericardiocentesis. Employing objective biomarkers, such as HRV, enhances the reliability of the findings and provides valuable insights into the physiological and psychological impact of these educational tools.
A key strength of this work lies in the cost-effective development of the training models, both of which were designed and implemented by the research team, including medical and biotechnology students, using widely accessible software and hardware. The affordability of the 3D-printed mannequin and VR system makes this approach highly scalable and adaptable for institutions with limited financial resources, thereby promoting the democratization of access to simulation-based training. By reducing the financial barriers associated with advanced simulators, this study highlights a pathway for integrating innovative educational tools in diverse educational settings. By incorporating feedback from clinical experts during the validation process, this study ensures the clinical and educational relevance of the models, thereby setting a benchmark for future simulation-based research. The findings underscore the potential of VR as an effective and accessible training tool, particularly in resource-limited settings or when traditional training methods are impractical. Additionally, the study’s implications extend beyond medical students in their final year, offering a framework that can be adapted for other learner groups and procedures of varying complexity. Finally, the open accessibility of the VR model via GitHub promotes reproducibility and encourages further innovation in the development of simulation-based training tools.
Future research should prioritize evaluating the generalizability of these findings across diverse learner populations, such as first-year medical students, residents, and practicing healthcare professionals. Exploring how stress responses vary with levels of clinical experience and expertise could inform the design of tailored simulation programs that address specific training needs. In addition, broadening the scope of the analyzed procedures is essential for understanding the versatility of the simulation tools. Although this study focused on pericardiocentesis, future research could investigate stress responses in simulations of less invasive procedures, such as venipuncture, or highly dynamic interventions, including trauma resuscitation and advanced cardiac life support. Such studies would help to elucidate how stress dynamics differ across clinical scenarios with varying levels of complexity and urgency. Advancing the technological features of VR simulations is another promising direction for future research. Integrating haptic feedback and real-time biometric monitoring can significantly enhance the realism and educational value of VR environments. Evaluating the impact of these advancements on both stress induction and skill acquisition will provide a more nuanced understanding of how to optimize VR for medical training. Finally, longitudinal studies are needed to assess how repeated exposure to simulation-based training influences long-term stress management, skill retention, and clinical performance. Understanding the evolution of stress responses over time and their correlation with improved coping mechanisms could help to establish evidence-based guidelines for incorporating simulation into medical curricula. These studies provide valuable insights into how simulation training shapes not only technical competence but also emotional resilience in healthcare professionals.
link





![Locum tenens offers physicians a path to freedom [PODCAST] Locum tenens offers physicians a path to freedom [PODCAST]](https://kevinmd.com/wp-content/uploads/Design-4-scaled.jpg)
