Impact of a virtual reality-based simulation training for shoulder dystocia on human and technical skills among caregivers: a randomized-controlled trial

Study design, setting, and ethical statements
This prospective, case–control, single-blind, 1:1 randomized crossover study (Fig. 2) was performed at the Obstetric Unit of our University Hospital, between January and August 2022. The study was conducted in accordance with the Declaration of Helsinki and the good clinical practice. The Data Protection Commission of the Medical University of Vienna (Datenschutzkommission der MedUni Wien) approved the clinical trial, and the institutional ethics committee of the Medical University of Vienna issued a waiver of approval. All participants provided written informed consent for enrolment in the study. This trial has been registred in the publicly accessible primary register with the registration number ISRCTN12194978 04/08/2023. This manuscript was structured according to the CONSORT 2010 checklist for randomized controlled trials.
Participants and recruitment
We contacted all eligible study participants via email and invited them to participate voluntarily in the SD training. Potential study participants included resident and attending physicians, midwives, and medical students in their final year of medical school; these personnel listed were considered eligible for study inclusion and randomization. An important prerequisite for the eligibility for the study was a theoretical understanding of the maneuvers needed to solve a shoulder dystocia scenario. Study participants were informed about the objectives of the study, signed an informed consent form, and completed the validated HuFSHI questionnaire to explore their critical self-reflection before and after training5.
Study groups, randomization, and blinding
A blinded sub-investigator at the Obstetric Unit of our University Hospital performed blocked simple randomization with a 1:1 allocation ratio and randomly varying block size. Participants signed an informed consent form and were allocated to either a study group (360° video played on a VR device) or a control group (frontal theoretical lesson via PowerPoint presentation). Sealed envelopes containing information about random allocation to the study (360° video played on a VR device) or control groups (frontal instruction) were supplied according to the randomization sequence. The 360°-VR video scenario for the study participants is described in detail below. For the control group, the second trainer gave a brief lecture on SD management describing 1:1 the shoulder dystocia scenario shown in the 360° video using a PowerPoint presentation (Microsoft, Redmond, Washington, United States) for 2 min and 50 s. Participants in the control group were allowed to ask questions; however, didactic teaching was not allowed. Thus, the trainer did not answer the participants ‘questions directly but tried to create an interactive learning environment to encourage self-directed learning’. The trial envelopes were safely stored at the study site and opened by the trainers during the first training day, allowing participants to be allocated. Each participant completed the HuFSHI, a 14-item questionnaire with a 1–10 Likert scale to assess human factor skills within healthcare providers (Supplemental Material 1)5. The HELPERR (H: call for help, E: consider episiotomy, L: legs, P: suprapubic pressure, E: enter maneuvers, R: remove the posterior arm, R: roll onto all fours) mnemonic formula, developed by the Advanced Life Support in Obstetrics (ALSO) providers, can be useful during acute SD management. According to local standards15, the Gaskin Maneuver (R) was anticipated and performed in cases where “L” (Mc Roberts maneuver) and “P” (suprapubic pressure) were unsuccessful. Therefore, the HELPERR mnemonic formula was modified for the HELP-RER (H: “call for help”, E: “consider episiotomy”, L: “legs”, P: “suprapubic pressure”, R: “rotate onto all fours”, E: “enter maneuvers”, R: “remove the posterior arm”) checklist, as shown in Fig. 1. The taught content was identical and did not differ between the groups. After training, each participant completed the NASA Task-Load Index (TLX) 6, a 6-item questionnaire with a 1 to 21 Likert scale to assess subjective workload during practical training (Supplemental Material 1). The participants and trainers were not blinded to the type of intervention or to the HELP-RER evaluation based on the nature of the study. The principal investigator was blinded to the type of intervention and did not participate in training. The outcome parameters (HuFSHI and TLX, time needed to solve the task, and HELP-RER algorithm score) were documented by the trainers at the end of the first training as HuFSHI(1), Time (1) TLX(1), and HELP-RER(1), and at the end of the second training (HuFSHI(2), time (2) TLX(2), and HELP-RER(2) (Fig. 2).

The HELP-RER mnemonic formula, modified from Baxley and Gobbo32.
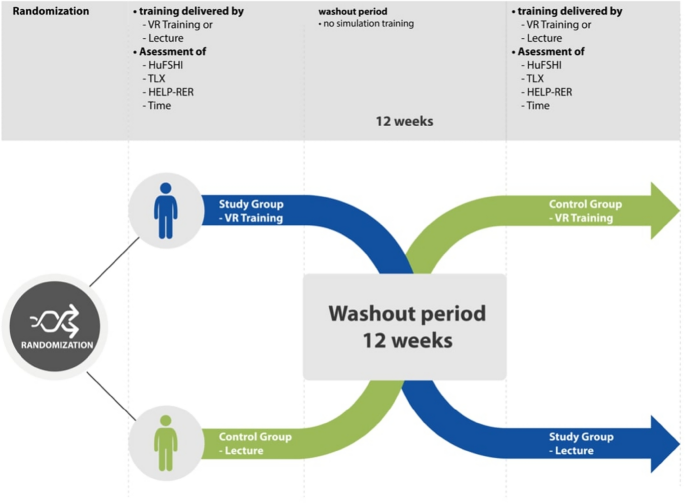
Study design of the prospective case–control, single-blinded, 1:1 randomized cross-over study, involving 61 participants among resident and consultant physicians, midwives and medical students during their final year of medical school.
The 360°-VR scenario
All training sessions were conducted in the delivery room of the Obstetric Unit of our University Hospital. An immersive 360°-VR scenario was developed to explore all obstetrical maneuvers needed to manage shoulder dystocia and lasted for 2 min and 50 s. The scenario was scripted and approved by a group of experts in the field of obstetrics and produced using a GoPro Max 360 camera (GoPro, San Mateo, California, US) remaining central in the room, thus allowing the 360°fields of view to be accessible by each participant viewing in the Quest 2 VR headset (Meta, Menlo Park, California, US). This headset features a state-of-the-art 845 Snapdragon processor and 4k resolution at a 75-Hz refresh rate (Meta, Menlo Park, California, US). One of the main advantages of this device is its standalone feature, as there is no need to plug it into a computer or use any additional sensors while still offering the option to connect wirelessly to external devices for a live view. The participants in the 360°VR group were allowed to move freely within the delivery room to enhance their immersive VR experience.
The script of the VR scenario was as follows: A 35-year-old female, Grav 1 Para 0, 160 cm, 85 kg, who had a spontaneous rupture of membranes and regular contractions in gestational week 40 + 2, was presented in the delivery room. She reported an uneventful pregnancy, except for gestational diabetes (treated with lifestyle modifications). According to the last fetal biometry performed at 36 + 0 weeks of gestation, fetal weight was estimated to be at the 70th percentile. Oxytocin infusion was initiated at a cervical dilation of 7 cm. Delivery was assisted by an experienced midwife and an obstetrical/gynecologist (ob/gyn) resident physician. After the delivery of the head, they observe the typical “turtle sign”, thereby defining shoulder dystocia. The resident physician immediately stopped the oxytocin infusion and called for help (H). The need for episiotomy (E) was also evaluated. Subsequently, they performed the McRoberts maneuver three times (L). A second midwife attempted to deliver the baby’s shoulder, but this was unsuccessful. The suprapubic pressure maneuver (P) was also unsuccessful. Subsequently, the obstetric team urged the patient to roll onto all four (R) in order to allow the delivery of the posterior shoulder. During the Gaskin maneuver (Fig. 3), a highly experienced attending physician arrived, and together with the midwife, they rolled the patient on her back to perform the Wood maneuver (E). The baby’s shoulder was delivered, and the baby was eventually transferred to the neonatology ward after immediate cord clamping.
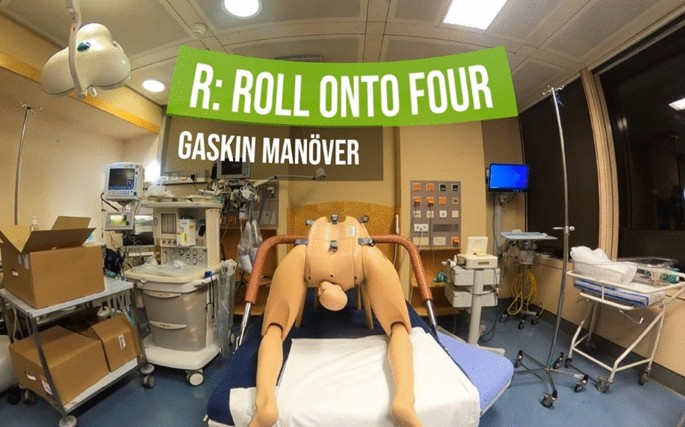
Example of an image shown during the 360° VR video training.
Assessment and outcomes
Following this first phase, each study participant underwent hands-on training on a high-fidelity PROMPT flex-advanced birth simulator manikin (Limbs and Things Ltd., Bristol, UK). Two different trainers noted the time needed to complete the task as well as the correct execution of the obstetrical maneuvers, as displayed in the modified ALSO algorithm HELP-RER(1). In particular, for each correctly performed letter on this checklist, the participants received one point. Thus, each participant reached a maximum score of 7 on the HELP-RER evaluation. In order to evaluate both short and long time retention through the two different training modalities, as well as to offer all participants both training modalities, each participant underwent alternative training (crossover) after a 12 weeks washout period16. HELP-RER scores were reassessed during hands-on training (HELP-RER(2)). The HuFSHI and TLX questionnaires were repeated (Fig. 2). The primary outcome of this study was the evaluation of adherence to the modified ALSO algorithm (HELP-RER) according to the training modality. The secondary outcomes were improvement in the diagnosis-to-delivery time, improvement in HuFSHI, and TLX scores after VR-based versus theory-based training. Further exploratory outcomes included the influence of clinical experience and training reiterations on the final scores.
Sample size calculation
There was no previous data on training effectiveness upon which to base our sample size calculation. We performed an a priori power analyses (with sample sizes per group ranging from 25 to 30), using the standard assumptions of power = 0.8 and significance levels of 0.05. Hence, a sample size of 32 per intervention was estimated to fit for this assumption.
Statistical methods
Quantitative variables are presented as the median and interquartile range (IQR), whereas categorical variables are reported as numbers and percentages (%). Associations between numerical outcomes were tested using the Wilcoxon rank-sum test. The chi-square test was used to compare the binary outcomes between participant groups. Statistical significance was set at p-values < 0.05 were considered statistically significant. To correct possible confounders, linear regressions with HELP-RER(2) as a dependent variable was performed to investigate the association between higher HELP-RER(2) scores after shoulder dystocia training and the following variables with a potential influence on the outcome: HELP-RER(1), years of clinical expertise, group, and education. For the model without HELP-RER(1), we computed an Akaike information criterion (AIC) of 117.52 vs. an AIC of 116.1 for the full model. Statistical analyses were performed using R software version 4.1.3 (R Development Core Team, Boston, MA, USA)17 and the packages pwr18 and ggplot219.
Role of the funding source
This research received no specific grant from any funding agency.
link





![Locum tenens offers physicians a path to freedom [PODCAST] Locum tenens offers physicians a path to freedom [PODCAST]](https://kevinmd.com/wp-content/uploads/Design-4-scaled.jpg)
